Tue, Jul 8, 2025
Volume 18, Issue 2 (Summer & Autumn 2021)
ASJ 2021, 18(2): 66-71 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
S. Ominde B, S. Igbigbi P. Variant Morphology of the Crista Galli in Adult Nigerians: A CT Study. ASJ 2021; 18 (2) :66-71
URL: http://anatomyjournal.ir/article-1-276-en.html
URL: http://anatomyjournal.ir/article-1-276-en.html
1- Department of Human Anatomy and Cell Biology, School of Basic Medical Sciences, Delta State University, Abraka, Nigeria.
Full-Text [PDF 569 kb]
(1613 Downloads)
| Abstract (HTML) (2052 Views)
Full-Text: (5083 Views)
1. Introduction
The crista galli is a thick triangular bone that originates from the superior surface of the ethmoid bone and perpendicularly projects into the anterior cranial fossa. Its thin and slightly curved posterior border anchors the falx cerebri of the dura mater [1]. The development of the crista galli begins at the eighth week of intrauterine life when the presphenoidal cartilage forms the mesethmoid cartilage, which forms the anterior skull base, including the cartilaginous crista galli. After birth, the ossification of crista galli starts at two months of age and rapidly increases until 14 months. Later, ossification slows down and ends by the second year of life [2, 3].
The crista galli may be pneumatized following the extension of air cells from adjacent paranasal sinuses, hence, it is called sinus crista galli [4]. Owing to its origin from the ethmoid bone, the crista galli may get aerated by displaced ethmoidal air cells [2]. Also, the extension of the aeration of the frontal sinus beyond the margins of the frontal bone may cause pneumatization of the crista galli [4]. This variant is important to clinicians since the obstruction of its drainage may lead to chronic sinusitis that is not amenable to medical therapy [5].
Moreover, the crista galli is important to surgeons since it acts as an important landmark during endoscopic sinus and skull base surgeries [4]. Its proximity with olfactory nerves that enter the cribriform foramina, the orbital content, and the anterior cranial fossa increases the risk of iatrogenic complications, such as cerebrospinal fluid leakage and the loss of vision or olfaction [6]. Besides, mucoceles from the crista galli may extend intracranially increasing risk for inadvertent intracranial penetration during surgery [3]. There is a paucity of data regarding the morphology of the crista galli in Delta State, Nigeria. Therefore, this study aimed to determine the morphological variants of the crista galli in adult Nigerians, using Computed Tomography (CT).
2. Materials and Methods
This retrospective study was conducted at the Radiology Department of Delta State University Teaching Hospital, Nigeria. The hospital’s Research and Ethics Committee granted ethical approval before the commencement of the study (Code: EREC/PAN/2020/030/0371). Brain CT images of 336 adult patients (199 males and 137 females) aged between 20 and 99 years were utilized. These were CT images taken between June 1, 2015, to June 30, 2020, using a 64-slice CT scanner and stored in the Picture Archiving and Communications software. We excluded the images of patients aged below 20 years and images with evidence of facial trauma, sinonasal pathologies, and previous sinus surgery. Then, the age and gender of the patients were documented. The crista galli was identified on the coronal section and its position was classified based on its relationship with the cribriform plate [6]. The type I crista galli had its base located at the level of the cribriform plate. However, less than 50% of the height of the crista galli was located below the level of the cribriform plate in type II, while type III included those with more than 50% of the height below the level of the plate. The crista galli was also studied for any extent of pneumatization.
Data were analyzed using SPSS v. 23, classified by gender, and summarized in frequencies. A chi-squared test was used to evaluate gender differences in the prevalence of these variants. Also, a P value of less than 0.05 was considered statistically significant.
3. Results
This study evaluated the CT scan images of 336 patients consisting of 199 males (59.2%) and 137 females (40.8%). The age range of the patients was 20 to 99 years with a Mean±SD age of 53.29±18.18 years. The findings of this study revealed type II crista galli as the most prevalent type (n=257, 76.5%), followed by type I (n=59, 17.6%) and lastly type III (n=20, 6%). There was no statistically significant association between the type of crista galli and gender (P=0.367, 0.146, and 0.281 for types I, II, and III, respectively) (Table 1 and Figure 1).
.png)
.png)
Table 2 shows a comparison of the types of crista galli in different populations.
.png)
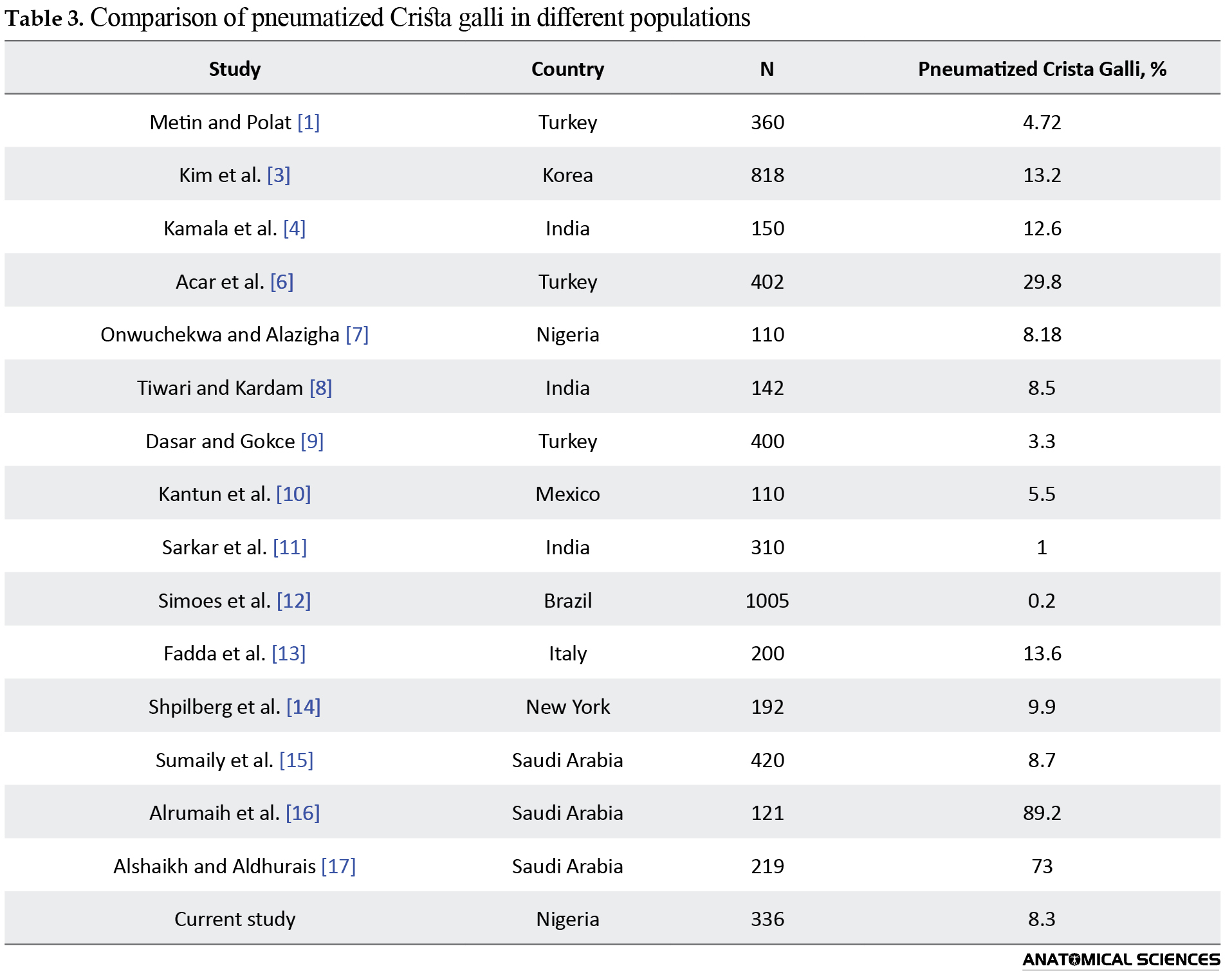
The pneumatization of the crista galli was observed in 28 patients (8.3%) with a slightly lower frequency in females (n=9, 6.6%) than in males (n=19, 9.5%). However, the gender difference was statistically insignificant (P=0.332). Moreover, pneumatization commonly occurred in type I (n=18, 64.3%), followed by type II (n=10, 35.7%). No pneumatization was observed in the type III crista galli (Figure 2). Table 3 shows the comparison of pneumatized crista galli in different populations.
4. Discussion
In the present study, the predominant type of crista galli was type II, followed by type I, and lastly, type III. Various studies in literature documented a similar pattern [3, 4, 6]. The prevalence of type II crista galli was 76.5%; this was lower than the prevalence rates of 84.2% and 82.5% reported by Kim et al. [3] and Kamala et al. [4] in Korea and India, respectively. However, Acar et al. [6] documented a lower prevalence of 64.9% in Turkey. Also, type I had a frequency of 17.6% that was higher than the frequencies of 13.9% and 12.5% reported by Kim et al. [3] and Kamala et al. [4], respectively. However, a slightly higher prevalence of 18.3% was reported among the Turkish population [6]. Type III was observed in 6% of the patients, which was comparable to the prevalence rate of 5% reported by Kamala et al. [4] and higher than 1.8% documented by Kim et al. [3]. Acar et al. [6] reported a prevalence of 16.8% that was higher than our findings. The discrepancies in the prevalence of the different types of crista galli in different studies have been ascribed to the differences in the sample size, methodology, ethnicity, and race [6].
The pneumatized crista galli had a prevalence of 8.3% that was comparable to the rates of 8.18% and 8.5% documented by Onwuchekwa and Alazigha [7] and Tiwari and Kardam [8] in Rivers State, Nigeria, and India, respectively. However, Dasar and Gokce [9], Metin and Polat [1], and Kantun et al. [10] documented the lower frequencies of 3.3%, 4.72%, and 5.5%, respectively, in Turkey and Mexico. Accordingly, very low prevalences of 1% and 0.2% were reported in India and Brazil [11, 12]. Nevertheless, the prevalences in Italy, Korea, New York, and India, documented by Fadda et al. [13], Kim et al. [3], Shpilberg et al. [14], and Kamala et al. [4], respectively, were slightly higher than in our study sample. According to literature reports, the pneumatized crista galli has shown a wide range of prevalence in Saudi Arabia. Akin to our findings, Sumaily et al. [15] documented a frequency of 8.7%. Contrarily, Alrumaih et al. [16] and Alshaikh and Aldhurais [17] documented a higher prevalence of 89.2% and 73%, respectively (Table 3). Metin and Polat [1] attributed the discrepancies in literature to differences in sample size, the anatomic definition of the variant, race, sex, age, and CT evaluation skills.
Our findings revealed a higher prevalence of pneumatization in the type I crista galli (64.3%), followed by type II (35.7%); none of the type III cases were pneumatized. Similarly, Acar et al. [6] observed sinus crista galli mostly in type I (37.8%) and type II (31.4%). Moreover, a small proportion of the pneumatized crista galli (14.9%) was observed among their patients with type III crista galli; this difference could be ascribed to race.
The awareness of the morphological variants of the crista galli aids radiologists, neurosurgeons, and otorhinolaryngologists in the evaluation of CT images preoperatively [5]. The recognition of the pneumatized crista galli is important since it can lead to frontal sinusitis, mucocele, and nasal dermoid formation [4]. They may also act as possible anatomical barriers during surgical resection of anterior cranial fossa tumors [6]. Sinus crista galli may be mistaken for an ethmoidal cell; this predisposes to an inadvertent invasion of the skull base during endoscopic sinus surgery [17].
5. Conclusion
In conclusion, the prevalence of the types of crista galli and its pneumatization in this study differed from some literature reports. Hence, the need for radiologists, otorhinolaryngologists, and neurosurgeons to recognize these variants during CT evaluation in our population.
Ethical Considerations
Compliance with ethical guidelines
Ethical approval was granted by the Hospital’s Research and Ethics Committee before the commencement of the study (Code: EREC/PAN/2020/030/0371).
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Conceptualization, Methodology, Funding acquisition: Beryl S. Ominde; Data collection and Data analysis: Patrick Igbigbi.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
We would like to acknowledge Priscilla Ejiroghene and Emmanuel Akpoyibo who assisted with data collection and analysis.
References
The crista galli is a thick triangular bone that originates from the superior surface of the ethmoid bone and perpendicularly projects into the anterior cranial fossa. Its thin and slightly curved posterior border anchors the falx cerebri of the dura mater [1]. The development of the crista galli begins at the eighth week of intrauterine life when the presphenoidal cartilage forms the mesethmoid cartilage, which forms the anterior skull base, including the cartilaginous crista galli. After birth, the ossification of crista galli starts at two months of age and rapidly increases until 14 months. Later, ossification slows down and ends by the second year of life [2, 3].
The crista galli may be pneumatized following the extension of air cells from adjacent paranasal sinuses, hence, it is called sinus crista galli [4]. Owing to its origin from the ethmoid bone, the crista galli may get aerated by displaced ethmoidal air cells [2]. Also, the extension of the aeration of the frontal sinus beyond the margins of the frontal bone may cause pneumatization of the crista galli [4]. This variant is important to clinicians since the obstruction of its drainage may lead to chronic sinusitis that is not amenable to medical therapy [5].
Moreover, the crista galli is important to surgeons since it acts as an important landmark during endoscopic sinus and skull base surgeries [4]. Its proximity with olfactory nerves that enter the cribriform foramina, the orbital content, and the anterior cranial fossa increases the risk of iatrogenic complications, such as cerebrospinal fluid leakage and the loss of vision or olfaction [6]. Besides, mucoceles from the crista galli may extend intracranially increasing risk for inadvertent intracranial penetration during surgery [3]. There is a paucity of data regarding the morphology of the crista galli in Delta State, Nigeria. Therefore, this study aimed to determine the morphological variants of the crista galli in adult Nigerians, using Computed Tomography (CT).
2. Materials and Methods
This retrospective study was conducted at the Radiology Department of Delta State University Teaching Hospital, Nigeria. The hospital’s Research and Ethics Committee granted ethical approval before the commencement of the study (Code: EREC/PAN/2020/030/0371). Brain CT images of 336 adult patients (199 males and 137 females) aged between 20 and 99 years were utilized. These were CT images taken between June 1, 2015, to June 30, 2020, using a 64-slice CT scanner and stored in the Picture Archiving and Communications software. We excluded the images of patients aged below 20 years and images with evidence of facial trauma, sinonasal pathologies, and previous sinus surgery. Then, the age and gender of the patients were documented. The crista galli was identified on the coronal section and its position was classified based on its relationship with the cribriform plate [6]. The type I crista galli had its base located at the level of the cribriform plate. However, less than 50% of the height of the crista galli was located below the level of the cribriform plate in type II, while type III included those with more than 50% of the height below the level of the plate. The crista galli was also studied for any extent of pneumatization.
Data were analyzed using SPSS v. 23, classified by gender, and summarized in frequencies. A chi-squared test was used to evaluate gender differences in the prevalence of these variants. Also, a P value of less than 0.05 was considered statistically significant.
3. Results
This study evaluated the CT scan images of 336 patients consisting of 199 males (59.2%) and 137 females (40.8%). The age range of the patients was 20 to 99 years with a Mean±SD age of 53.29±18.18 years. The findings of this study revealed type II crista galli as the most prevalent type (n=257, 76.5%), followed by type I (n=59, 17.6%) and lastly type III (n=20, 6%). There was no statistically significant association between the type of crista galli and gender (P=0.367, 0.146, and 0.281 for types I, II, and III, respectively) (Table 1 and Figure 1).
.png)
.png)
Table 2 shows a comparison of the types of crista galli in different populations.
.png)
The pneumatization of the crista galli was observed in 28 patients (8.3%) with a slightly lower frequency in females (n=9, 6.6%) than in males (n=19, 9.5%). However, the gender difference was statistically insignificant (P=0.332). Moreover, pneumatization commonly occurred in type I (n=18, 64.3%), followed by type II (n=10, 35.7%). No pneumatization was observed in the type III crista galli (Figure 2). Table 3 shows the comparison of pneumatized crista galli in different populations.

4. Discussion
In the present study, the predominant type of crista galli was type II, followed by type I, and lastly, type III. Various studies in literature documented a similar pattern [3, 4, 6]. The prevalence of type II crista galli was 76.5%; this was lower than the prevalence rates of 84.2% and 82.5% reported by Kim et al. [3] and Kamala et al. [4] in Korea and India, respectively. However, Acar et al. [6] documented a lower prevalence of 64.9% in Turkey. Also, type I had a frequency of 17.6% that was higher than the frequencies of 13.9% and 12.5% reported by Kim et al. [3] and Kamala et al. [4], respectively. However, a slightly higher prevalence of 18.3% was reported among the Turkish population [6]. Type III was observed in 6% of the patients, which was comparable to the prevalence rate of 5% reported by Kamala et al. [4] and higher than 1.8% documented by Kim et al. [3]. Acar et al. [6] reported a prevalence of 16.8% that was higher than our findings. The discrepancies in the prevalence of the different types of crista galli in different studies have been ascribed to the differences in the sample size, methodology, ethnicity, and race [6].
The pneumatized crista galli had a prevalence of 8.3% that was comparable to the rates of 8.18% and 8.5% documented by Onwuchekwa and Alazigha [7] and Tiwari and Kardam [8] in Rivers State, Nigeria, and India, respectively. However, Dasar and Gokce [9], Metin and Polat [1], and Kantun et al. [10] documented the lower frequencies of 3.3%, 4.72%, and 5.5%, respectively, in Turkey and Mexico. Accordingly, very low prevalences of 1% and 0.2% were reported in India and Brazil [11, 12]. Nevertheless, the prevalences in Italy, Korea, New York, and India, documented by Fadda et al. [13], Kim et al. [3], Shpilberg et al. [14], and Kamala et al. [4], respectively, were slightly higher than in our study sample. According to literature reports, the pneumatized crista galli has shown a wide range of prevalence in Saudi Arabia. Akin to our findings, Sumaily et al. [15] documented a frequency of 8.7%. Contrarily, Alrumaih et al. [16] and Alshaikh and Aldhurais [17] documented a higher prevalence of 89.2% and 73%, respectively (Table 3). Metin and Polat [1] attributed the discrepancies in literature to differences in sample size, the anatomic definition of the variant, race, sex, age, and CT evaluation skills.
Our findings revealed a higher prevalence of pneumatization in the type I crista galli (64.3%), followed by type II (35.7%); none of the type III cases were pneumatized. Similarly, Acar et al. [6] observed sinus crista galli mostly in type I (37.8%) and type II (31.4%). Moreover, a small proportion of the pneumatized crista galli (14.9%) was observed among their patients with type III crista galli; this difference could be ascribed to race.
The awareness of the morphological variants of the crista galli aids radiologists, neurosurgeons, and otorhinolaryngologists in the evaluation of CT images preoperatively [5]. The recognition of the pneumatized crista galli is important since it can lead to frontal sinusitis, mucocele, and nasal dermoid formation [4]. They may also act as possible anatomical barriers during surgical resection of anterior cranial fossa tumors [6]. Sinus crista galli may be mistaken for an ethmoidal cell; this predisposes to an inadvertent invasion of the skull base during endoscopic sinus surgery [17].
5. Conclusion
In conclusion, the prevalence of the types of crista galli and its pneumatization in this study differed from some literature reports. Hence, the need for radiologists, otorhinolaryngologists, and neurosurgeons to recognize these variants during CT evaluation in our population.
Ethical Considerations
Compliance with ethical guidelines
Ethical approval was granted by the Hospital’s Research and Ethics Committee before the commencement of the study (Code: EREC/PAN/2020/030/0371).
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Conceptualization, Methodology, Funding acquisition: Beryl S. Ominde; Data collection and Data analysis: Patrick Igbigbi.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
We would like to acknowledge Priscilla Ejiroghene and Emmanuel Akpoyibo who assisted with data collection and analysis.
References
- Metin-Tellioglu A, Polat Y. The incidence of sinus crista galli in children and adults. A computerized tomography study. International Journal of Morphology. 2019; 37(2):735-8. [DOI:10.4067/S0717-95022019000200735]
- Som PM, Park EE, Naidich TP, Lawson W. Crista galli pneumatization is an extension of the adjacent frontal sinuses. American Journal of Neuroradiology. 2009; 30(1):31-3. [DOI:10.3174/ajnr.A1291] [PMID] [PMCID]
- Kim JJ, Cho JH, Choi JW, Lim HW, Song YJ, Choi SJ, et al. Morphologic analysis of crista galli using computed tomography. Journal of Rhinology. 2012; 19(2):91-5. https://www.j-rhinology.org/upload/pdf/jr-19-2-91.pdf
- Kamala E, Vijaya SU, Gugapriya TS, kumar NV. A computerized tomographic study of morphology and pneumatization of crista galli. International Journal of Anatomy and Research. 2016; 4(2):2429-33. [DOI:10.16965/ijar.2016.227]
- Tetiker H, Kosar MI, Çullu N, Sahan M, Gençer CU, Derin S. Pneumatization of crista galli in pre-adult and adult stages. International Journal of Morphology. 2016; 34(2):541-4. [DOI:10.4067/S0717-95022016000200021]
- Acar G, Cicekcibasi AE, Koplay M, Kelesoglu KS. The relationship between the pneumatization patterns of the frontal sinus, crista galli and nasal septum: A tomography study. Turkish Neurosurgery. 2020; 30(4):532-41. [DOI:10.5137/1019-5149.JTN.26006-19.4] [PMID]
- Onwuchekwa RC, Alazigha N. Computed tomography anatomy of the paranasal sinuses and anatomical variants of clinical relevants in Nigerian adults. Egyptian Journal of Ear, Nose, Throat and Allied Sciences. 2017; 18(1):31−8. [DOI:10.1016/j.ejenta.2016.11.001]
- Tiwari TN, Kardam NK. CT evaluation of anatomical variations of paranasal sinus region and their clinical importance. International Journal of Research in Medical Sciences. 2019; 7(6):2260-4. [DOI:10.18203/2320-6012.ijrms20192509]
- Dasar U, Gokce E. Evaluation of variations in sinonasal region with computed tomography. World Journal of Radiology. 2016; 8(1):98-108. [DOI:10.4329/wjr.v8.i1.98] [PMID] [PMCID]
- Kantun JAS, Acosta MEH, Campo MCA, Rivera DEN, Oceguera LM, Silva JD. Anatomical variations of paranasal sinuses in patients with chronic sinusitis. International Journal of Radiology & Radiation Therapy. 2019; 6(5):186-9. https://medcraveonline.com/IJRRT/IJRRT-06-00244.pdf
- Sarkar PS, Bhosale PR, Bharthi AR, Ananthasivan R. Computed tomography scan correlation between anatomic variations of paranasal sinuses and chronic rhinosinusitis. International Journal of Scientific Study. 2016; 4(4):122-8. https://scholar.google.com/scholar?q=+Computed+Tomography+scan+correlation+between+anatomic+variations+of+paranasal+sinuses+and+chronic+rhinosinusitis&hl=fa&as_sdt=0,5
- Simoes NM, Cameiro PMR, Silva AIV, de Souza PEA, Manzi.FR. Anatomic variation of paranasal sinuses. Journal of Oral Diagnosis. 2017; 2:e20170038. [DOI:10.5935/2525-5711.20170038]
- Fadda GL, Rosso S, Aversa S, Petrelli A, Ondolo C, Succo G. Multiparametric statistical correlations between paranasal sinus anatomic variations and chronic rhinosinusitis. Acta Otorhinolaryngologica Italica. 2012; 32(4):244-51. [PMID] [PMCID]
- Shpilberg KA, Daniel SC, Doshi AH, Lawson W, Som PM. CT of anatomic variants of the paranasal sinuses and nasal cavity: Poor correlation with radiologically significant rhinosinusitis but importance in surgical planning. American Journal of Roentgenology. 2015; 204(6):1255-60. [DOI:10.2214/AJR.14.13762] [PMID]
- Sumaily I, Aldhabaan S, Hudise J. Anatomical variations of paranasal sinuses gender and age impact. Global Journal of Otolaryngology. 2018; 14(1):555877. [DOI:10.19080/GJO.2018.14.555877]
- Alrumaih RA, Ashoor MM, Obidan AA, Al-Khater KM, Al-Jubran SA. Radiological sinonasal anatomy. Exploring the Saudi population. Saudi Medical Journal. 2016; 37(5):521-6. [DOI:10.15537/smj.2016.5.13904] [PMID] [PMCID]
- Alshaikh N, Aldhurais A. Anatomic variations of the nose and paranasal sinuses in Saudi population: Computed tomography scan analysis. The Egyptian Journal of Otolaryngology. 2018; 34(4):234-41. [DOI:10.4103/1012-5574.244904]
Type of Study: Original |
Subject:
Gross Anatomy
Received: 2021/03/24 | Accepted: 2021/06/23 | Published: 2021/09/28
Received: 2021/03/24 | Accepted: 2021/06/23 | Published: 2021/09/28
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |




.png)
