Fri, Jul 4, 2025
Volume 19, Issue 2 (Summer & Autumn 2022)
ASJ 2022, 19(2): 111-118 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Ahrabi B, Noroozian M, Taheri-Panah R, Nazarian H, Fadaee Fathabadi F, Alaee S, et al . Effect of Adriamycin on α1β1, α1β4, and ανβ3 Expression in Rat Endometrium in Estrus Phase. ASJ 2022; 19 (2) :111-118
URL: http://anatomyjournal.ir/article-1-588-en.html
URL: http://anatomyjournal.ir/article-1-588-en.html
Behnaz Ahrabi1 

 , Mohsen Noroozian2
, Mohsen Noroozian2 
 , Robabeh Taheri-Panah1
, Robabeh Taheri-Panah1 
 , Hamid Nazarian2
, Hamid Nazarian2 

 , Fatemeh Fadaee Fathabadi2
, Fatemeh Fadaee Fathabadi2 
 , Sanaz Alaee3
, Sanaz Alaee3 

 , Marefat Ghaffari Novin1
, Marefat Ghaffari Novin1 

 , Hojjat-Allah Abbaszadeh4
, Hojjat-Allah Abbaszadeh4 




 , Mohsen Noroozian2
, Mohsen Noroozian2 
 , Robabeh Taheri-Panah1
, Robabeh Taheri-Panah1 
 , Hamid Nazarian2
, Hamid Nazarian2 

 , Fatemeh Fadaee Fathabadi2
, Fatemeh Fadaee Fathabadi2 
 , Sanaz Alaee3
, Sanaz Alaee3 

 , Marefat Ghaffari Novin1
, Marefat Ghaffari Novin1 

 , Hojjat-Allah Abbaszadeh4
, Hojjat-Allah Abbaszadeh4 


1- Infertility and Reproductive Health Research Center (IRHRC), Shahid Beheshti University of Medical Sciences, Tehran, Iran.
2- Department of Biology and Anatomical Sciences, School of Medicine, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
3- Department of Reproductive Biology, School of Advanced Medical Sciences and Technologies, Shiraz University of Medical Sciences, Shiraz, Iran.
4- Hearing Disorders Research Center, Loghman Hakim Hospital, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
2- Department of Biology and Anatomical Sciences, School of Medicine, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
3- Department of Reproductive Biology, School of Advanced Medical Sciences and Technologies, Shiraz University of Medical Sciences, Shiraz, Iran.
4- Hearing Disorders Research Center, Loghman Hakim Hospital, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
Full-Text [PDF 703 kb]
(277 Downloads)
| Abstract (HTML) (1954 Views)
Full-Text: (240 Views)
1. Introduction
Chemotherapy is an essential process for treating people with cancer. As awareness of the side effects of breast cancer chemotherapy increases in terms of reproduction, many breast cancer patients are seeking strategies to maintain their fertility [1]. Although aggressive chemotherapy improves the lives of women with cancer during their reproductive years, the effect on the ovaries usually results in infertility. So far, several studies have been carried out on changes in ovarian reserve, endocrine function, and MIS hormones (Mullerian inhibiting factor, LH, follicle-stimulating hormone, estradiol, and menstrual status) in young women with breast cancer under chemotherapy [2]. It has also been demonstrated that women who have had chemotherapy before menopause are more likely to develop amenorrhea and impaired fertility [1]. Other side effects of chemotherapy include the reduction of AMH hormone, anti-mullerian hormone, and inhibin B, degradation of primary follicles, a decrease in antral follicles, ovarian volume, and ovarian atrophy [2]. An effective chemotherapy drug for the treatment of cancer is adriamycin (doxorubicin), one of the strongest antibiotic anthracycline drugs extracted from Streptomyces peucetius var, which is used to treat malignant sarcoma, lung cancer, neuroblastoma, and breast cancer. Acute and chronic cardiotoxicity associated with the dose induced by this drug has limited its use. Endometriosis undergoes morphologic changes during implantation, and in this phase, minor changes occur in the nucleus and mitochondria, the rough endoplasmic network, and the vascular system [3]. The implantation of the fetus in the mother’s uterus depends on two factors: The quality of the fetus and the quality of the endometrium. Integrins are one of the most important factors that play a vital role during implantation. Up until now, there have been many types of integrin that have remained known, but three types are expressed during implantation: α1β1, α4β1, and ανβ3 [2]. Epithelial integrin ανβ3 is expressed at the epithelial endometrial surface on days 19-24 of menstrual cycles. Previous research has found that the amount of this integrin expressed during the luteal phase is reduced in LPD, endometriosis, and infertility due to unspecified and hydrosalpinx [4]. The integrin molecules α1β1, α4β1, and ανβ3 are considered to evaluate the potential for endometrial admission in the implantation phase and are all expressed together. The expression of structural integrin α2, α3, α6, and β4 is expressed uniformly in all healthy endometrium. The subunits α2 and α3 are expressed in total cells, whereas α6 and β4 are localized at the lateral surface of the endometrial glands [5]. Steroid hormones play an important role in the appearance and in regulating the expression of integrins in the secretion phase. α1β1 is a receptor of laminin and collagen, and progesterone can directly increase its expression in the endometrial secretion phase [5-7]. ανβ3 integrins appear in the endometrial epithelium at 19-20 cycles. Three amino acids of Arg-gly-asp are detected in this integrin, which is effective in the endometrial binding of trophoblast [7]. and its expression in the endometrium depends on endometrial puberty and sexual hormones are capable of affecting this expression [8]. Pregnancy in rodents like mice is based on the Estrous cycle because mating and pregnancy occur only in the estrus phase. Given the importance of the role of α1β1, α4β1, and ανβ3 integrins in the implantation, it is expected that the expression of integrins α1β1, α4β1, and ανβ3 genes in chemotherapy in the estrous phase be different. The aim of the present study was to determine the effect of adriamycin on the expression of 1β1α, 1β4α, and νβ3α integrin genes in the endometrial tissue of adult female rats in the estrous phase. Given the effect of adriamycin, the purpose of the present study was to evaluate the effect of adriamycin on the expression of integrin genes.
2. Methods
Animals
An experimental study was performed on 32 three-month-old Wistar female rats with a weight of 180–200 g, prepared by the Pasteur Institute of Tehran. Animals were kept at the central animal house of Shahid Beheshti University of Medical Sciences, Tehran, at 24°C, 12 h of light, and 12 h of darkness, and fed with special rodent food. After adapting the animals to their new environment, they were randomly divided into four groups (sham, control, and experiment with adriamycin at 4 mg/kg and 8 mg/kg doses for 6 weeks), with eight animals in each group.
Adriamycin injection method
The experimental group received 4 and 8 mg/kg of adriamycin (with 10 mg of vial, American Pharmacia Company) via intraperitoneal (i.p.) injection for 4 weeks, each time 0.5 mL (one time per week). The dose is equal to the recommended dose for the treatment of breast cancer in rats [4]. Subsequently, mice were evaluated 2 weeks after injection, and their mortality was calculated.
Determining the stage of the estrus cycle
Female rats have a 4–5-day cycle of estrus. The estrous phase was determined for each adult rat using a vaginal smear test. The estrous phase was determined by the proportion of cells in the smear after crystal violet staining. A vaginal smear cytology was performed in one of the four stages of proestrus, metestrus, estrous, and diestrous. A vaginal smear was prepared early morning to ensure the rats had the same cycle. In this method, 50 μL of distilled water was piped into the animal’s vagina and then placed on a slide. After drying, the sample was stained with crystal violet. After being stained, the specimens were detected using an optical microscope with a magnification of 40, and the stages of the estrous cycle were determined based on the classical cellular characteristics of the specimens so that in the estrus stage, surface cells were without nuclei and foamy [9] (Figure 1).
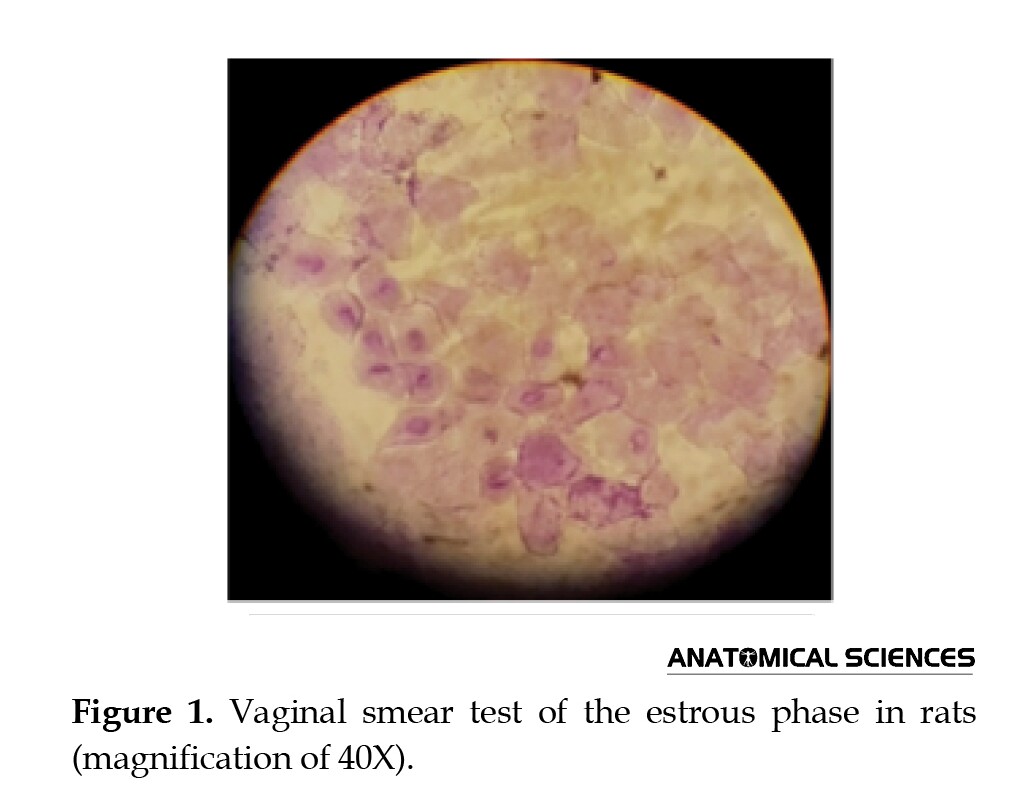
Sample preparation
After determining the stage of the estrous phase, eight rats were randomly divided into three groups: Control, experiment, and sham. The rats were then sacrificed by dislocation of the cervical vertebrae. A tissue sample of about 2 mL was prepared from 1/3 of the uterus for real-time PCR. Samples were washed with a high volume of buffer. The endometrial tissue was removed and frozen at -20°C in a microtube containing RNA later.
Real-time polymerase chain reaction analysis (RT-PCR)
At first, the samples were crushed. RNA extraction kit was used to extract RNA (Yekta Tajhiz Azma, Iran) according to the manufacturer’s protocol. Prime Script™ RT Reagent Kit (Fermentas, Canada) was used to synthesize cDNA. The cDNA synthesis reaction was carried out at 42°C for 60 minutes and stored at -20°C. All real-time PCR reactions were performed on the Roche machine. The temperature schedule for the device was set in three steps: The first stage causes the denaturation of cDNA molecules (95°C for 10 min). The second stage was 60°C for 30 s of annealing and 30 s at 72°C in 40 consecutive cycles. Finally, the third step was 10 min at 72°C for extension. The primer sequences used for RT-PCR are summarized in Table 1. Relative cartilage gene expression was analyzed using the comparative Ct method (2−ΔΔCt).

3. Results
Animal weight and mortality rate
Two weeks after the last injection of adriamycin, the survival rate was 100% in the control group, but in the group treated with adriamycin, the highest dose was 8 mg/kg to 0%, and a dose of 4 mg reduced the weight of the rats. The average weight of the animals in the experimental group with a dose of 4 mg/kg (3.12±19.19) was lower than that of the control group (7.27±14.26). There was a significant difference between the control and treatment groups with adriamycin in terms of weight (P<0.05) (Table 2, Figure 2).
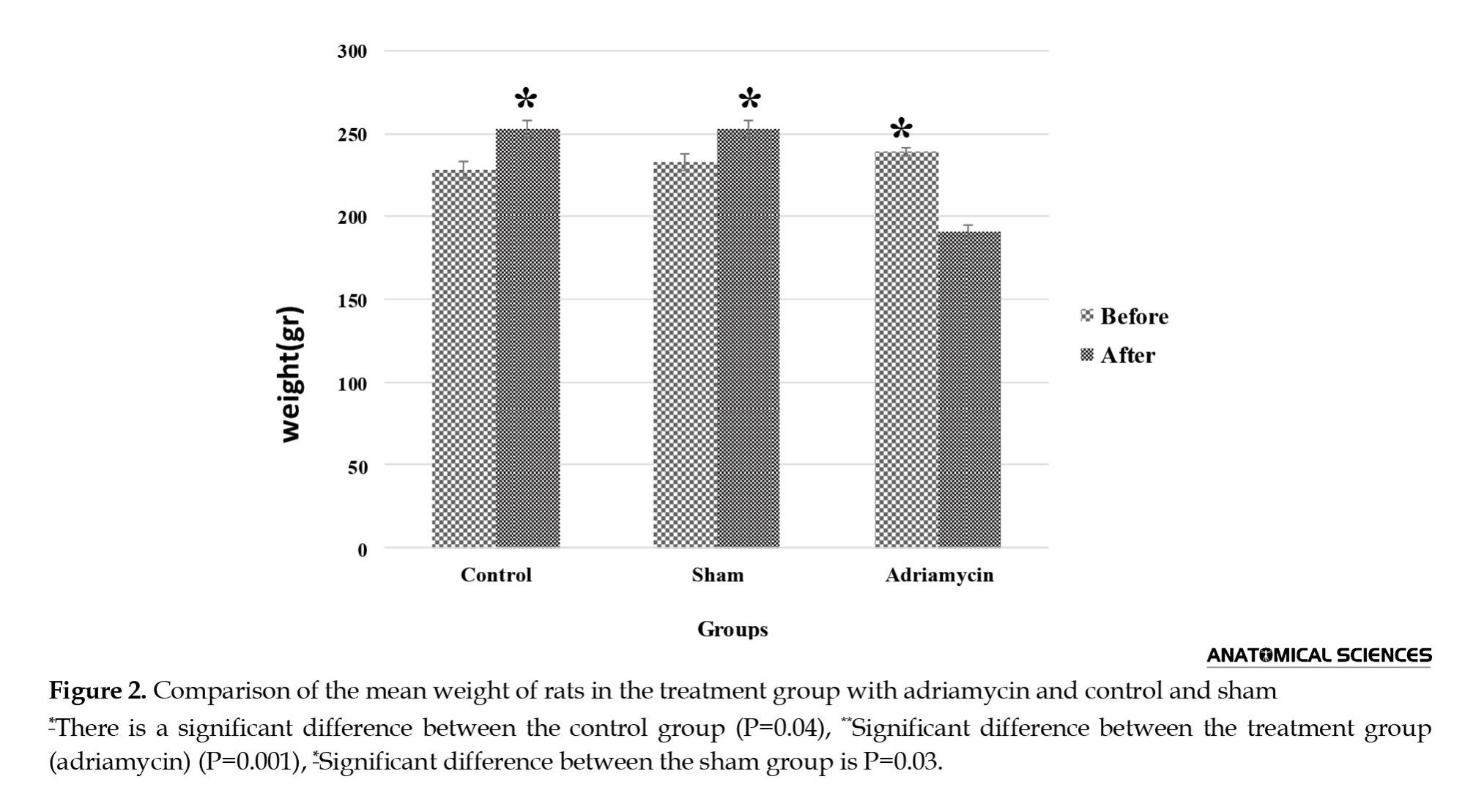
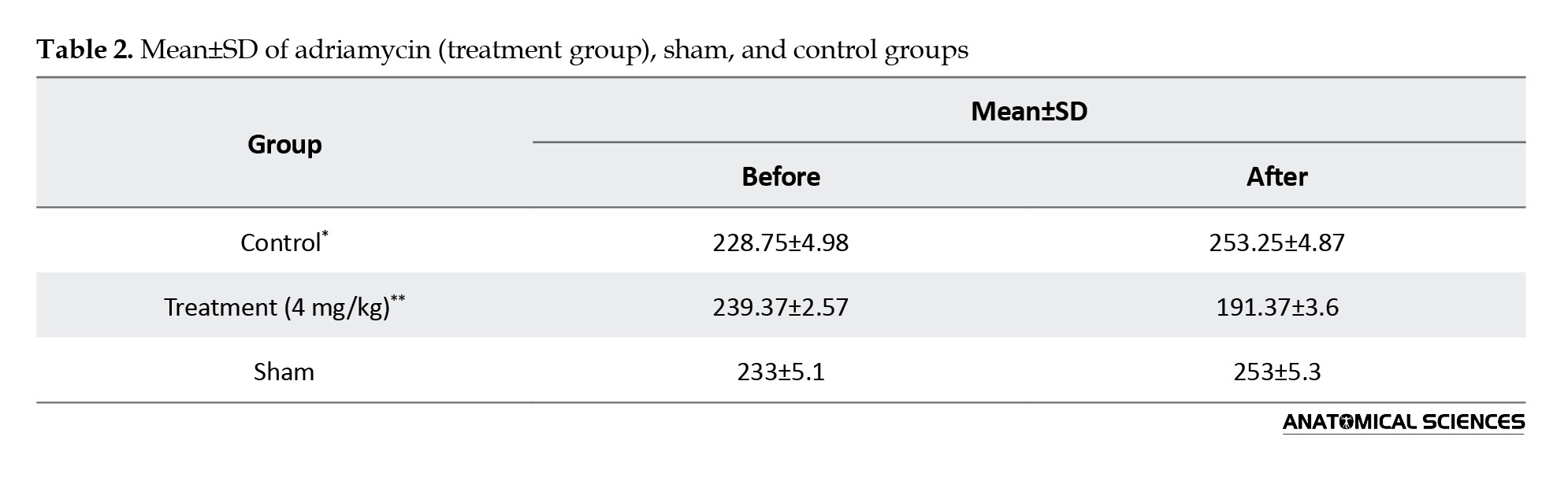
Integrin gene expression level
Estrus stage was determined based on the classical cellular characteristics of the specimens two weeks after the last adriamycin injection, and endometrial samples of uterine rats were collected and evaluated for Integrin gene expression level using the real-time PCR technique. Also, the rate of expression of integrin α1 in the treated group was not significantly different from those of the control and sham groups (P>0.05) (Figure 3, Table 3).


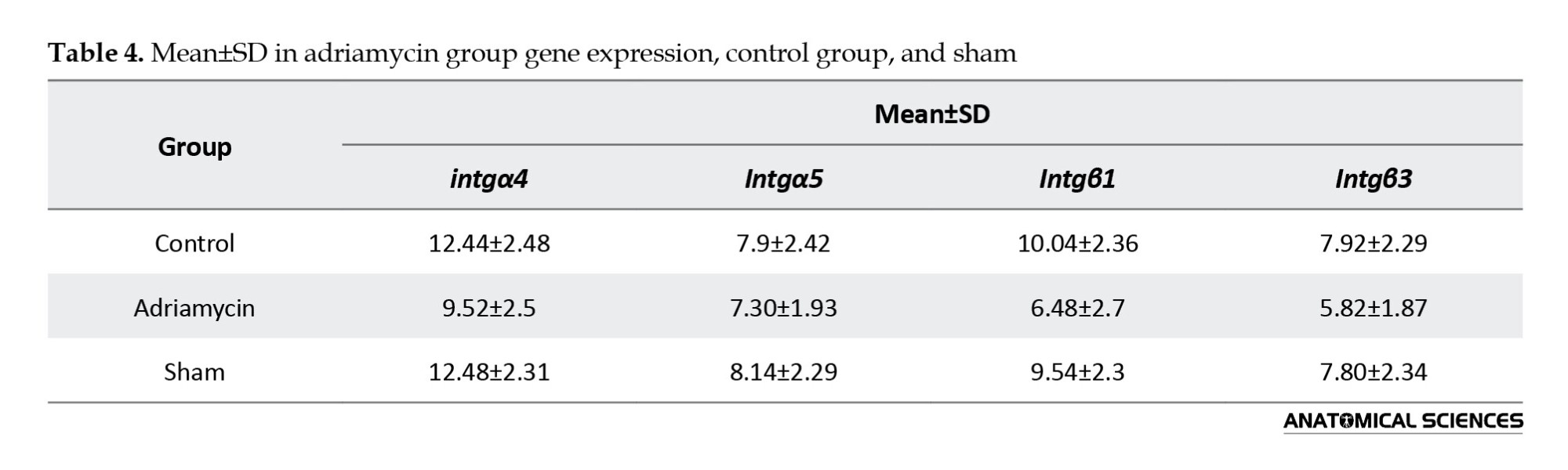
Moreover, the results showed that there was no significant difference in the expression of integrin genes α4 and β3 between the treated groups (adriamycin group) and those of the sham and control groups (Figure 3); however, the level of intgα1 expression in the treated group with adriamycin was significantly increased as compared to the control group (P<0.05, Value=0.027) (Figure 3). The results showed that there was no significant difference in intgβ1 gene expression between the adriamycin group, sham group, and control group (P>0.05) (Figure 4, Table 4).
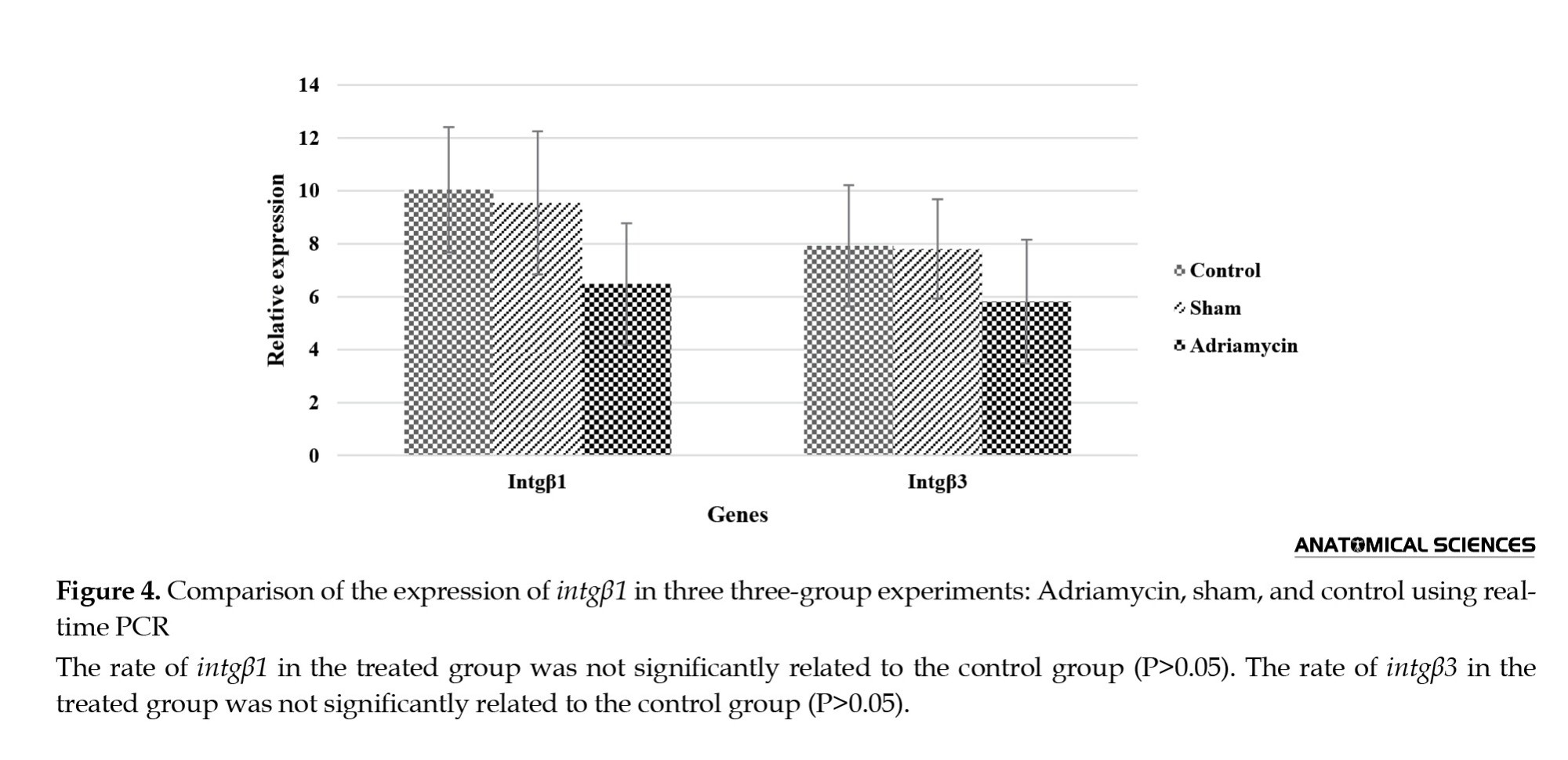
In the current study, injection of adriamycin into rats significantly increased the expression of the intgα1 gene in the endometrium as compared to intgαᵥ, intgβ1, intgβ3, and intgα4.
4. Discussion
Although aggressive chemotherapy improves the lives of women at reproductive age with breast cancer, it frequently results in infertility, ovarian damage, and ovarian cancer. Three chemotherapeutic drugs, adriamycin, taxol, and cyclophosphamide, are used in the literature to treat breast cancer, from which adriamycin was used in the present study [10]. Ottewell and his colleagues (2008) used adriamycin at doses of 2 mg/kg, 4 mg/kg, and 8 mg/kg for breast cancer treatment. Their research showed that the dose of 8 mg/kg was effective in improving cancer patients compared to the other two doses [11]. However, in the present study, this dose was known as a toxic dose due to the high mortality rate at a dose of 8 mg/kg.
According to recent studies by other researchers, it can be concluded that one of the reasons for weight loss is vomiting and lack of appetite, which can be due to the stimulation of chemical receptors on the bottom of the ventricle located in the medulla. In the present study, intraperitoneal administration of adriamycin for 6 weeks at a dose of 4 mg/kg significantly reduced the rats’ weight, consistent with the findings reported by Tei et al. (2003) [12]. According to the results of the present study, there was no significant difference in the expression of integrin genes β1, α4, αᵥ, and β3 except α1 between the treated groups with adriamycin and the control group. Thomas et al. (2002) investigated the stimulation of gonadotropins on α1β1, α4β1, and ανβ3 expression using the immunohistochemistry method, which reduced expression in all three integrins in glandular epithelium and decreased αββ3 expression in luminal epithelium. Regarding the significant effect of the expression of these integrins on the implantation phase and the stimulatory effect of gonadotropins in IVF, a reduction of the expression of these integrins was observed [7]. In another study, immunohistochemistry was used to assess the expression of ανβ3 integrin during the implantation phase in 10 fertile women and 22 women with infertility of unknown cause. In this study, patients with infertility, due to an unknown reason, had lower levels of ανβ3 integrin expression [13]. However, in our study, using Real Time-PCR, the gene expressions of the treatment group with adriamycin, β1, β3, α5, and α4 were found to be different compared with those of the control group. In addition, the expression of α1 was upregulated in the adriamycin group. Peyghambari et al. conducted a study on the expression changes of β3, αv, β1, and α4 and osteopontin ligands in the phases of the sexual cycle in 15 rat rats. Because binding of integrins to the extracellular matrix requires a specific ligand such as collagen 4, fibronectin, laminin, and osteopontin, immunohistochemistry results showed that expression of β3, αv, β1, α4, and β4 was only in the met estrus stage. Among these Specific ligands, osteopontin is one of the extracellular matrix molecules found in most organisms secreted in the osteopontin genital system by endometrial secretion cells, invasive trophoblasts. This study also determined that osteopontin is secreted by progesterone from the uterine gland and that its ligand is ανβ3 [14]. In the study mentioned above, the expression of integrin genes is considered to be in the met estrus stage, while in our study, the expression of integrin α1 gene with real-time PCR was positive only in the estrus stage as a result of injection of adriamycin. According to a study by Yang et al. (1999), who examined the expression of osteopontin mRNA with different concentrations of doxorubicin in the breast cancer cell model using Western blotting and RT PCR, it can be concluded that the osteopontin ligand can be effective in increasing the expression of integrin α1 [15]. In the present study, the increased expression of α1 inhibition in the estrus phase was higher than that of other integrins, which may be one of the reasons for its increase in the expression of the osteopontin ligand.
Vernaeve et al. (2007) investigated donated ovum implantation in women who had a history of developing a variety of cancers, including breast cancer and Hodgkin’s lymphoma sarcoma, who were treated with chemotherapy, and compared the results with those without any history of the disease. The results showed that chemotherapy during the implantation of donated oocytes had no effect on people who had previously been co-treated with chemotherapy [15]. While in our study, the expression of integrin genes that play an important role in endometrial receptors was evaluated, no significant difference was found in the expression of integrin genes of α4, αν, β3, and β1 in the control and experimental groups.
The results of this study corresponded to those reported by Vernaeve et al. (2007), who used adriamycin chemotherapy in the implantation phase. Due to the complications of chemotherapy and infertility, many fertility patients who are planning to have a pregnancy have fertility assistance options, such as egg cultures, donated eggs, or even fetal storage, until after the completion of chemotherapy and return of the menstrual cycle, when pregnancy occurs through IVF or other ways. But the point to consider is whether endometrial admission is maintained after the end of the chemotherapy period. According to a study by Vernaeve et al. (2007) on the effect of chemotherapy on endometrial receptors after oocyte donation in cancer patients, chemotherapy had no effect on oocyte susceptibility, and there was no significant difference in endometrial receptor in chemotherapy patients and in the control group that had oocyte donation [15].
5. Conclusions
Chemotherapy with adriamycin has no effect on integrin α4, α5, β3, and β1 receptors and can even increase the expression of the α1 endometrial receptor gene. Consequently, for young women who have cancer at fertility age, there is a hope that after the completion of chemotherapy and returning to a menstrual cycle, even in the absence of ovarian reserve, they can experience pregnancy and childbirth with the help of assisted reproductive techniques.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles are considered in this article.
Funding
This research was funded by School of Medicine, Shahid Beheshti University of Medical Sciences.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors are thankful of School of Medicine, Shahid Beheshti University of Medical Sciences, for the fund.
References
Chemotherapy is an essential process for treating people with cancer. As awareness of the side effects of breast cancer chemotherapy increases in terms of reproduction, many breast cancer patients are seeking strategies to maintain their fertility [1]. Although aggressive chemotherapy improves the lives of women with cancer during their reproductive years, the effect on the ovaries usually results in infertility. So far, several studies have been carried out on changes in ovarian reserve, endocrine function, and MIS hormones (Mullerian inhibiting factor, LH, follicle-stimulating hormone, estradiol, and menstrual status) in young women with breast cancer under chemotherapy [2]. It has also been demonstrated that women who have had chemotherapy before menopause are more likely to develop amenorrhea and impaired fertility [1]. Other side effects of chemotherapy include the reduction of AMH hormone, anti-mullerian hormone, and inhibin B, degradation of primary follicles, a decrease in antral follicles, ovarian volume, and ovarian atrophy [2]. An effective chemotherapy drug for the treatment of cancer is adriamycin (doxorubicin), one of the strongest antibiotic anthracycline drugs extracted from Streptomyces peucetius var, which is used to treat malignant sarcoma, lung cancer, neuroblastoma, and breast cancer. Acute and chronic cardiotoxicity associated with the dose induced by this drug has limited its use. Endometriosis undergoes morphologic changes during implantation, and in this phase, minor changes occur in the nucleus and mitochondria, the rough endoplasmic network, and the vascular system [3]. The implantation of the fetus in the mother’s uterus depends on two factors: The quality of the fetus and the quality of the endometrium. Integrins are one of the most important factors that play a vital role during implantation. Up until now, there have been many types of integrin that have remained known, but three types are expressed during implantation: α1β1, α4β1, and ανβ3 [2]. Epithelial integrin ανβ3 is expressed at the epithelial endometrial surface on days 19-24 of menstrual cycles. Previous research has found that the amount of this integrin expressed during the luteal phase is reduced in LPD, endometriosis, and infertility due to unspecified and hydrosalpinx [4]. The integrin molecules α1β1, α4β1, and ανβ3 are considered to evaluate the potential for endometrial admission in the implantation phase and are all expressed together. The expression of structural integrin α2, α3, α6, and β4 is expressed uniformly in all healthy endometrium. The subunits α2 and α3 are expressed in total cells, whereas α6 and β4 are localized at the lateral surface of the endometrial glands [5]. Steroid hormones play an important role in the appearance and in regulating the expression of integrins in the secretion phase. α1β1 is a receptor of laminin and collagen, and progesterone can directly increase its expression in the endometrial secretion phase [5-7]. ανβ3 integrins appear in the endometrial epithelium at 19-20 cycles. Three amino acids of Arg-gly-asp are detected in this integrin, which is effective in the endometrial binding of trophoblast [7]. and its expression in the endometrium depends on endometrial puberty and sexual hormones are capable of affecting this expression [8]. Pregnancy in rodents like mice is based on the Estrous cycle because mating and pregnancy occur only in the estrus phase. Given the importance of the role of α1β1, α4β1, and ανβ3 integrins in the implantation, it is expected that the expression of integrins α1β1, α4β1, and ανβ3 genes in chemotherapy in the estrous phase be different. The aim of the present study was to determine the effect of adriamycin on the expression of 1β1α, 1β4α, and νβ3α integrin genes in the endometrial tissue of adult female rats in the estrous phase. Given the effect of adriamycin, the purpose of the present study was to evaluate the effect of adriamycin on the expression of integrin genes.
2. Methods
Animals
An experimental study was performed on 32 three-month-old Wistar female rats with a weight of 180–200 g, prepared by the Pasteur Institute of Tehran. Animals were kept at the central animal house of Shahid Beheshti University of Medical Sciences, Tehran, at 24°C, 12 h of light, and 12 h of darkness, and fed with special rodent food. After adapting the animals to their new environment, they were randomly divided into four groups (sham, control, and experiment with adriamycin at 4 mg/kg and 8 mg/kg doses for 6 weeks), with eight animals in each group.
Adriamycin injection method
The experimental group received 4 and 8 mg/kg of adriamycin (with 10 mg of vial, American Pharmacia Company) via intraperitoneal (i.p.) injection for 4 weeks, each time 0.5 mL (one time per week). The dose is equal to the recommended dose for the treatment of breast cancer in rats [4]. Subsequently, mice were evaluated 2 weeks after injection, and their mortality was calculated.
Determining the stage of the estrus cycle
Female rats have a 4–5-day cycle of estrus. The estrous phase was determined for each adult rat using a vaginal smear test. The estrous phase was determined by the proportion of cells in the smear after crystal violet staining. A vaginal smear cytology was performed in one of the four stages of proestrus, metestrus, estrous, and diestrous. A vaginal smear was prepared early morning to ensure the rats had the same cycle. In this method, 50 μL of distilled water was piped into the animal’s vagina and then placed on a slide. After drying, the sample was stained with crystal violet. After being stained, the specimens were detected using an optical microscope with a magnification of 40, and the stages of the estrous cycle were determined based on the classical cellular characteristics of the specimens so that in the estrus stage, surface cells were without nuclei and foamy [9] (Figure 1).

Sample preparation
After determining the stage of the estrous phase, eight rats were randomly divided into three groups: Control, experiment, and sham. The rats were then sacrificed by dislocation of the cervical vertebrae. A tissue sample of about 2 mL was prepared from 1/3 of the uterus for real-time PCR. Samples were washed with a high volume of buffer. The endometrial tissue was removed and frozen at -20°C in a microtube containing RNA later.
Real-time polymerase chain reaction analysis (RT-PCR)
At first, the samples were crushed. RNA extraction kit was used to extract RNA (Yekta Tajhiz Azma, Iran) according to the manufacturer’s protocol. Prime Script™ RT Reagent Kit (Fermentas, Canada) was used to synthesize cDNA. The cDNA synthesis reaction was carried out at 42°C for 60 minutes and stored at -20°C. All real-time PCR reactions were performed on the Roche machine. The temperature schedule for the device was set in three steps: The first stage causes the denaturation of cDNA molecules (95°C for 10 min). The second stage was 60°C for 30 s of annealing and 30 s at 72°C in 40 consecutive cycles. Finally, the third step was 10 min at 72°C for extension. The primer sequences used for RT-PCR are summarized in Table 1. Relative cartilage gene expression was analyzed using the comparative Ct method (2−ΔΔCt).

3. Results
Animal weight and mortality rate
Two weeks after the last injection of adriamycin, the survival rate was 100% in the control group, but in the group treated with adriamycin, the highest dose was 8 mg/kg to 0%, and a dose of 4 mg reduced the weight of the rats. The average weight of the animals in the experimental group with a dose of 4 mg/kg (3.12±19.19) was lower than that of the control group (7.27±14.26). There was a significant difference between the control and treatment groups with adriamycin in terms of weight (P<0.05) (Table 2, Figure 2).


Integrin gene expression level
Estrus stage was determined based on the classical cellular characteristics of the specimens two weeks after the last adriamycin injection, and endometrial samples of uterine rats were collected and evaluated for Integrin gene expression level using the real-time PCR technique. Also, the rate of expression of integrin α1 in the treated group was not significantly different from those of the control and sham groups (P>0.05) (Figure 3, Table 3).


Moreover, the results showed that there was no significant difference in the expression of integrin genes α4 and β3 between the treated groups (adriamycin group) and those of the sham and control groups (Figure 3); however, the level of intgα1 expression in the treated group with adriamycin was significantly increased as compared to the control group (P<0.05, Value=0.027) (Figure 3). The results showed that there was no significant difference in intgβ1 gene expression between the adriamycin group, sham group, and control group (P>0.05) (Figure 4, Table 4).

In the current study, injection of adriamycin into rats significantly increased the expression of the intgα1 gene in the endometrium as compared to intgαᵥ, intgβ1, intgβ3, and intgα4.

4. Discussion
Although aggressive chemotherapy improves the lives of women at reproductive age with breast cancer, it frequently results in infertility, ovarian damage, and ovarian cancer. Three chemotherapeutic drugs, adriamycin, taxol, and cyclophosphamide, are used in the literature to treat breast cancer, from which adriamycin was used in the present study [10]. Ottewell and his colleagues (2008) used adriamycin at doses of 2 mg/kg, 4 mg/kg, and 8 mg/kg for breast cancer treatment. Their research showed that the dose of 8 mg/kg was effective in improving cancer patients compared to the other two doses [11]. However, in the present study, this dose was known as a toxic dose due to the high mortality rate at a dose of 8 mg/kg.
According to recent studies by other researchers, it can be concluded that one of the reasons for weight loss is vomiting and lack of appetite, which can be due to the stimulation of chemical receptors on the bottom of the ventricle located in the medulla. In the present study, intraperitoneal administration of adriamycin for 6 weeks at a dose of 4 mg/kg significantly reduced the rats’ weight, consistent with the findings reported by Tei et al. (2003) [12]. According to the results of the present study, there was no significant difference in the expression of integrin genes β1, α4, αᵥ, and β3 except α1 between the treated groups with adriamycin and the control group. Thomas et al. (2002) investigated the stimulation of gonadotropins on α1β1, α4β1, and ανβ3 expression using the immunohistochemistry method, which reduced expression in all three integrins in glandular epithelium and decreased αββ3 expression in luminal epithelium. Regarding the significant effect of the expression of these integrins on the implantation phase and the stimulatory effect of gonadotropins in IVF, a reduction of the expression of these integrins was observed [7]. In another study, immunohistochemistry was used to assess the expression of ανβ3 integrin during the implantation phase in 10 fertile women and 22 women with infertility of unknown cause. In this study, patients with infertility, due to an unknown reason, had lower levels of ανβ3 integrin expression [13]. However, in our study, using Real Time-PCR, the gene expressions of the treatment group with adriamycin, β1, β3, α5, and α4 were found to be different compared with those of the control group. In addition, the expression of α1 was upregulated in the adriamycin group. Peyghambari et al. conducted a study on the expression changes of β3, αv, β1, and α4 and osteopontin ligands in the phases of the sexual cycle in 15 rat rats. Because binding of integrins to the extracellular matrix requires a specific ligand such as collagen 4, fibronectin, laminin, and osteopontin, immunohistochemistry results showed that expression of β3, αv, β1, α4, and β4 was only in the met estrus stage. Among these Specific ligands, osteopontin is one of the extracellular matrix molecules found in most organisms secreted in the osteopontin genital system by endometrial secretion cells, invasive trophoblasts. This study also determined that osteopontin is secreted by progesterone from the uterine gland and that its ligand is ανβ3 [14]. In the study mentioned above, the expression of integrin genes is considered to be in the met estrus stage, while in our study, the expression of integrin α1 gene with real-time PCR was positive only in the estrus stage as a result of injection of adriamycin. According to a study by Yang et al. (1999), who examined the expression of osteopontin mRNA with different concentrations of doxorubicin in the breast cancer cell model using Western blotting and RT PCR, it can be concluded that the osteopontin ligand can be effective in increasing the expression of integrin α1 [15]. In the present study, the increased expression of α1 inhibition in the estrus phase was higher than that of other integrins, which may be one of the reasons for its increase in the expression of the osteopontin ligand.
Vernaeve et al. (2007) investigated donated ovum implantation in women who had a history of developing a variety of cancers, including breast cancer and Hodgkin’s lymphoma sarcoma, who were treated with chemotherapy, and compared the results with those without any history of the disease. The results showed that chemotherapy during the implantation of donated oocytes had no effect on people who had previously been co-treated with chemotherapy [15]. While in our study, the expression of integrin genes that play an important role in endometrial receptors was evaluated, no significant difference was found in the expression of integrin genes of α4, αν, β3, and β1 in the control and experimental groups.
The results of this study corresponded to those reported by Vernaeve et al. (2007), who used adriamycin chemotherapy in the implantation phase. Due to the complications of chemotherapy and infertility, many fertility patients who are planning to have a pregnancy have fertility assistance options, such as egg cultures, donated eggs, or even fetal storage, until after the completion of chemotherapy and return of the menstrual cycle, when pregnancy occurs through IVF or other ways. But the point to consider is whether endometrial admission is maintained after the end of the chemotherapy period. According to a study by Vernaeve et al. (2007) on the effect of chemotherapy on endometrial receptors after oocyte donation in cancer patients, chemotherapy had no effect on oocyte susceptibility, and there was no significant difference in endometrial receptor in chemotherapy patients and in the control group that had oocyte donation [15].
5. Conclusions
Chemotherapy with adriamycin has no effect on integrin α4, α5, β3, and β1 receptors and can even increase the expression of the α1 endometrial receptor gene. Consequently, for young women who have cancer at fertility age, there is a hope that after the completion of chemotherapy and returning to a menstrual cycle, even in the absence of ovarian reserve, they can experience pregnancy and childbirth with the help of assisted reproductive techniques.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles are considered in this article.
Funding
This research was funded by School of Medicine, Shahid Beheshti University of Medical Sciences.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors are thankful of School of Medicine, Shahid Beheshti University of Medical Sciences, for the fund.
References
- Lund MJ, Brawley OP, Ward KC, Young JL, Gabram SS, Eley JW. Parity and disparity in first course treatment of invasive breast cancer. Breast Cancer Research and Treatment. 2008; 109(3):545-57. [DOI:10.1007/s10549-007-9675-8] [PMID]
- Anderson RA, Themmen AP, Al-Qahtani A, Groome NP, Cameron DA. The effects of chemotherapy and long-term gonadotrophin suppression on the ovarian reserve in premenopausal women with breast cancer. Human Reproduction. 2006; 21(10):2583-92. [DOI:10.1093/humrep/del201] [PMID]
- Sarani SA, Ghaffari-Novin M, Warren MA, Dockery P, Cooke ID. Morphological evidence for theimplantation window‘in human luminal endometrium. Human Reproduction. 1999; 14(12):3101-6. [DOI:10.1093/humrep/14.12.3101] [PMID]
- Gonzalez RR, Palomino A, Boric A, Vega M, Devoto L. A quantitative evaluation of α1, α4, αV and β3 endometrial integrins of fertile and unexplained infertile women during the menstrual cycle. A flow cytometric appraisal. Human Reproduction. 1999; 14(10): 2485-92. [DOI:10.1093/humrep/14.10.2485] [PMID]
- Lessey BA, Damjanovich L, Coutifaris C, Castelbaum A, Albelda SM, Buck CA. Integrin adhesion molecules in the human endometrium. Correlation with the normal and abnormal menstrual cycle. The Journal of Clinical Investigation. 1992; 90(1): 188-95. [DOI:10.1172/JCI115835] [PMID]
- Bischof P, Redard M, Gindre P, Vassilakos P, Campana A. Localization of alpha 2, alpha 5 and alpha 6 integrin subunits in human endometrium, decidua and trophoblast. European Journal of Obstetrics & Gynecology and Reproductive Biology. 1993; 51(3): 217-26. [PMID]
- Thomas K, Thomson AJ, Sephton V, Cowan C, Wood S, Vince G, et al. The effect of gonadotrophic stimulation on integrin expression in the endometrium. Human Reproduction. 2002; 17(1): 63-8. [PMID]
- Creus M, Balasch J, Ordi J, Fábregues F, Casamitjana R, Quinto L, et al. Integrin expression in normal and out-of-phase endometria. Human Reproduction. 1998; 13(12): 3460-8. [DOI:10.1093/humrep/13.12.3460] [PMID]
- Marcondes FK, Bianchi FJ, Tanno AP. Determination of the estrous cycle phases of rats: Some helpful considerations. Brazilian Journal of Biology. 2002; 62(4A):609-4. [DOI:10.1590/S1519-69842002000400008] [PMID]
- Saadati F, Mahdikia H, Abbaszadeh HA, Abdollahifar MA, Khoramgah MS, Shokri B. Comparison of direct and indirect cold atmospheric-pressure plasma methods in the B 16 F 10 melanoma cancer cells treatment. Scientific Reports . 2018; 8(1):7689 . [DOI:10.1038/s41598-018-25990-9] [PMID]
- Ottewell PD, Mönkkönen H, Jones M, Lefley DV, Coleman RE, Holen I. Antitumor effects of doxorubicin followed by zoledronic acid in a mouse model of breast cancer. Journal of the National Cancer Institute. 2008; 100(16):1167-78. [DOI:10.1093/jnci/djn240] [PMID]
- Tei C, Maruyama T, Kuji N, Miyazaki T, Mikami M, Yoshimura Y. Reduced expression of αvβ3 integrin in the endometrium of unexplained infertility patients with recurrent IVF-ET failures: Improvement by danazol treatment. Journal of Assisted Reproduction and Genetics. 2003; 20(1): 13-20. [DOI:10.1023/A:1021254620888] [PMID]
- Peyghambari F, Amanpour S, Fayazi M, Haddadi M, Muhammadnejad S, Muhammadnejad A, et a;. Expression of α4, αv, β1 and β3 integrins during the implantation window on blastocyst of a mouse model of polycystic ovarian syndromes. Iranian Journal of Reproductive Medicine. 2014; 12(9): 623-32. [PMID]
- Yang SZ, Kohno N, Kondo K, Yokoyama A, Hamada H, Hiwada K, et al. Adriamycin activates E-cadherin-mediated cell-cell adhesion in human breast cancer cells.International Journal of Oncology. 1999; 15(6):1109-15. [DOI:10.3892/ijo.15.6.1109] [PMID]
- Vernaeve V, Bodri D, Colodrón M, Vidal R, Durbán M, Coll O. Endometrial receptivity after oocyte donation in recipients with a history of chemotherapy and/or radiotherapy.Human Reproduction.2007; 22(11):2863-7. [DOI:10.1093/humrep/dem276] [PMID]
Type of Study: Original |
Subject:
Reproductive Biology
Received: 2022/03/10 | Accepted: 2022/05/15 | Published: 2022/07/1
Received: 2022/03/10 | Accepted: 2022/05/15 | Published: 2022/07/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |

